By Chris Healey
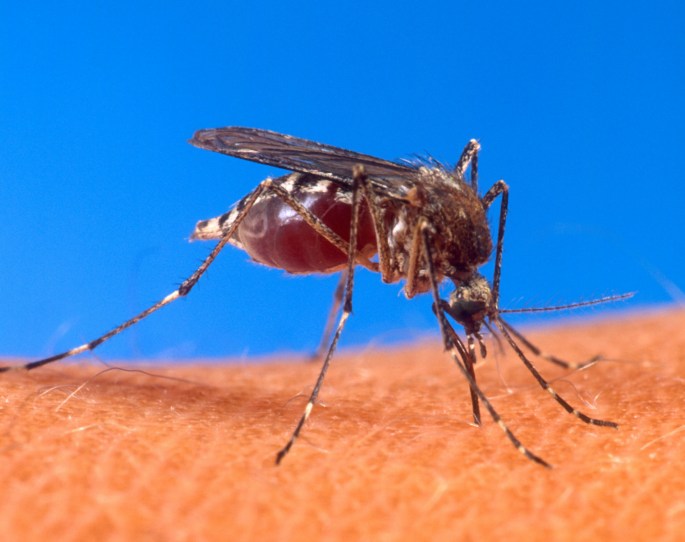
Mosquitos are responsible for a chickungunya fever outbreak in the Caribbean several hundred miles off the United States coastline. That outbreak is an addition to the expanding role arthropods play in the spread of illness.
Many arthropods are erroneously classified as insects. While mosquitos, lice, and fleas are indeed insects with six legs, ticks have eight legs and are technically arachnids. The term arthropod is an overarching classification encompassing mosquitos, fleas, and ticks – all common disease vectors. Insects are arthropods, but not all arthropods are insects.
Arthropods spread several of the world’s most significant diseases. Notable among them are Lyme disease, typhus, yellow fever, Japanese encephalitis, West Nile virus, and, most significantly, malaria. Of the 45 select agents designated by the U.S. Department of Health and Human Services, 12 are transmitted by arthropods.
Diseases spread by arthropods have influenced some of the greatest conflicts in history. More French soldiers are suspected to have died from louse-borne typhus than actual combat during Napoleon’s ill-fated 1812 invasion of Russia. Staggering mortality among the French army forced Napoleon to renounce Moscow and retreat back to France. During WWII, mosquito-borne malaria was a serious health threat to U.S troops throughout campaigns in the South Pacific.
Several tick-borne bacterial illnesses have been endemic to North America since antiquity, including Lyme disease and Rocky Mountain spotted fever. In recent years, mosquito-borne viruses have made their way across U.S. borders. The introduction of West Nile virus in 1999 and a 2005 dengue hemorrhagic fever outbreak in Texas have solidified emerging and foreign arthropod-borne diseases as threats to U.S. public health.
Arthropods can also serve to carry out bioterrorism. Terrorists could utilize arthropods to execute clandestine bioterror attacks through exploitation of feeding behavior. Inoculation of arthropods with the desired agent and subsequent release into unsuspecting populations could spread illness during, or shortly after, blood meals. Although possible, that scenario is unlikely due to the difficulty associated with production and maintenance of pathogen-inoculated arthropods.
A more likely bioterrorism scenario involves malevolent forces utilizing more passive means of compromising U.S. health. North America has many indigenous mosquito species – several of which can spread pathogens found in other parts of the world, such as Rift Valley Fever in Africa. Introduction of any disease capable of spread and maintenance by indigenous arthropods is a significant public health threat. Some unsubstantiated theories suggest West Nile virus was intentionally introduced to the U.S. in this way. Possibilities of an arthropod-facilitated attack has placed a heavy burden on keeping undesirable pathogens out of the country.
There are steps everyone can take to reduce their risk of arthropod-borne diseases. Mosquito control methods, such as elimination of outdoor untreated stagnant water sources, should be practiced regularly. Also, mosquito repellent, in addition to long-sleeved shirts and pants covering the ankles, should be worn whenever going outdoors.
Similar measures can be taken to prevent tick bites – wear repellent, tuck pants into socks or boots, shower after returning indoors, and perform tick checks daily.