Happy Friday Biodefense Gurus! We have a packed edition of the Pandora Report this week, but before we begin – don’t forget to register and reserve your spot for the “Coronavirus & International Security” panel event this evening in Arlington, VA. The CSPS Distinguished Speaker Series event will be at 5pm and you can find more information and register here.
 GMU Biodefense Summer Workshop on Pandemics, Bioterrorism, and Global Health Security
GMU Biodefense Summer Workshop on Pandemics, Bioterrorism, and Global Health Security
We’re excited to announce the summer dates for the workshop: Pandemics, Bioterrorism, and Global Health Security: From Anthrax to Zika. This three and a half-day workshop will be held in Arlington, VA, from July 13-16, 2020. Registration links and speaker information will be provided in the coming weeks. We hope you’ll join us for this immersive and engaging workshop with some of the top minds in the biodefense world, where we’ll discuss everything from synthetic biology to MCM, antibiotic resistance, and the current outbreak of COVID-19.
CW Use in Syria – Atrocities and Accountability
We’ve got the scoop on a brand new article by GMU Biodefense graduate program director and professor Dr. Gregory Koblentz in Nonproliferation Review regarding Assad regime use of chemical weapons. International efforts to hold the government of President Bashar al-Assad accountable for the use of chemical weapons in the Syrian civil war have entered a new phase. For the first time, the Organization for the Prohibition of Chemical Weapons (OPCW), the international organization responsible for implementing the 1993 Chemical Weapons Convention, has been empowered to identify the perpetrators of chemical attacks in Syria. The Investigation and Identification Team (IIT), which was formed to conduct the OPCW’s new attribution mission, has announced its intention to investigate and identify the perpetrators of nine chemical attacks in Syria, including the April 7, 2018, attack in Douma. This article reviews recent efforts to attribute chemical attacks in Syria, describes what we know about the nine incidents to be investigated, discusses what to expect during the next phase of the attribution process, and offers insights into how the international community can move beyond attribution to accountability. An annex to the article summarizes what is known about the Syrian government officials, military commanders, and chemical-warfare scientists suspected of being responsible for these attacks. As Koblentz notes, “Without attribution, there can be no accountability. Without accountability, the atrocities will continue: if not by the hand of Assad, then by others emboldened by his ability to use outlawed weapons to hold onto power.” You can read the article here, which builds upon his previous research on Syria’s chain of command for the use of chemical weapons and international efforts to hold the regime accountable for these attacks.
 Reaping What You Sow: The Case for Better Agroterrorism Preparedness
Reaping What You Sow: The Case for Better Agroterrorism Preparedness
GMU Biodefense MS student Stevie Kiesel is pulling back the curtain on this all too forgotten aspect of biodefense – agroterrorism. “An attack on the food supply gives the perpetrating group several benefits. First, the psychological and economic effect of targeting food supplies would be substantial. Such an effect could have a powerful pull with a group such as al Qaeda, who has shown interest in biological weapons and in targeting US economic strength. Second, and related, this type of attack would be relatively low cost when compared to the economic effects it could cause. Third, similar to other forms of terrorism, agroterrorism can allow a weaker group to lessen the power imbalance between themselves and the state they are targeting. Fourth, some groups may turn to agroterrorist tactics because these attacks ‘do not harm humans directly and may therefore be more easily justified’.” Read more of Stevie’s highly engaging and relevant article here.
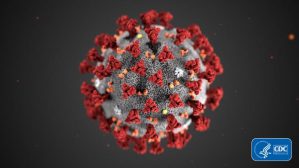
SARS-CoV-2/COVID-19 Outbreak Updates
As of Thursday evening, there have been 76,214 cases and 2,247 deaths related to COVID-19. From the realm of synthetic biology, many are rushing to recreate SARS-CoV-2 from its DNA code. Since it only took a few weeks to get the genetic sequence of the virus, many researchers are hoping to start ordering copies of genes to build it for efforts like diagnostic testing and vaccine development. On another front, one of the biggest topics has been that of cruise ships…One in particular, the MS Westerdam, finally docked and passengers/crew disembarked in Cambodia. Unfortunately, following the release of passengers, one was later found to have the disease, which has prompted concern as people have begun their travels home. The other, the Diamond Princess ship, finally saw its passengers allowed to leave the controversial ship-based quarantine. 621 (20% of the people onboard) of those on the ship tested positive for the virus. “Those passengers who have been declared free of the virus and are leaving the ship for the first time in two weeks face a confusing array of circumstances. Many will be forced to undergo a 14-day quarantine upon their return home — reflecting a lack of trust in the effectiveness of the ship’s quarantine. Others can remain in Japan under their own recognizance but are still barred from returning home for two weeks.” Here is a good timeline of the outbreak onboard and how the ship was initially placed into quarantine on February 4th after 10 people onboard tested positive. Passengers being flown back to the U.S. have been sharing their account of the experience, but as these two cruise ships provide unique examples of outbreak response, it sheds light on the limitations of quarantine and challenges of public health efforts during the COVID-19 outbreak. “Based on what is known so far, Cambodia’s approach is preferable to quarantining people aboard a ship where the virus is spreading, said Saskia V. Popescu, GMU Biodefense alum and senior infection prevention epidemiologist for HonorHealth, a hospital system in Phoenix. But that requires educating passengers about reporting symptoms and self-isolating if necessary, and having public health authorities in home countries closely monitor those who have returned. It includes quickly tracing the contacts of anyone who develops the infection. ‘I think we can say if you’re going to quarantine people, doing it on a cruise ship is not the best place,’ Popescu said.” In the face of these exhaustive efforts to respond to the disease, conspiracy theories have been a frustrating distraction – Chinese labs have noted that these often hurt efforts to curb the virus and scientists around the world have been working to condemn rumors and conspiracy theories regarding the origin of the virus. “A group of 27 prominent public health scientists from outside China is pushing back against a steady stream of stories and even a scientific paper suggesting a laboratory in Wuhan, China, may be the origin of the outbreak of COVID-19.” Senator Tom Cotton continues to push such conspiracy theories. The Federation of American Scientists (FAS) has a new initiative regarding the outbreak, known as the Coronavirus Project. The project focuses on debunking misinformation and providing accurate information from qualified researchers and scientists. “Since late 2019, information about the infectious Coronavirus has been trickling out from sources around the web. But not all information is created equal. Some of this information comes from science and medical professionals, who have years of experience in epidemiology. Some comes from unreliable anonymous internet accounts, bad actors, and hoaxers.” Despite these distractions, a paper in The Lancet recently emphasized the support for scientists, public health professionals, and medical professionals in China combatting the disease. “We have watched as the scientists, public health professionals, and medical professionals of China, in particular, have worked diligently and effectively to rapidly identify the pathogen behind this outbreak, put in place significant measures to reduce its impact, and share their results transparently with the global health community. This effort has been remarkable.” In times like these, the global health security community truly comes together to address common vulnerabilities and enhance strengths.
 The Economic Impacts of COVID-19
The Economic Impacts of COVID-19
The ongoing outbreak of coronavirus has already infected over 75,000 people and taken over 2,000 lives. The newly dubbed COVID-19 outbreak originated and remains strongest in China, but the economic effects of the it is already rippling across the globe. As an outbreak disseminates and intensifies, the labor force shrinks (at least temporarily), supply chains fracture, international mobility of persons and products decelerates or ceases altogether, and spending and investment decline. Though the full magnitude of economic effects from the outbreak can only be speculated upon at this point, the downward economic trends have begun. The sectors most impacted and at highest risk, thus far, are technology, oil, apparel, retail, tourism, and automobiles. The losses in production from Chinese manufacturing of key inputs and final products are critical drivers of the losses we are seeing and will continue to see across the globe. These items include iron, steel, aluminum, textiles, cement, chemicals, toys, electronics, and many more. According to the latest Statista Infographics Bulletin, global shipments of various tech products are expected to fall by 4.5 to 16% in this first quarter of the year. China is the world’s primary producer and exporter of textiles, so the fall in Chinese textile production will impact the global apparel and retail markets. Global oil demand is falling for the first time in over a decade as global transit drops from diminished trade and travel. Travel bans are, of course, squelching international tourism and costing travel hot spots to lose revenue. This is compounded as major events that attract troves of visitors are cancelled in response to COVID-19 fears. For instance, projections from the UN’s International Civil Aviation Organization expect Japan to lose $1.3 billion and Thailand to lose $1.2 billion in tourism revenue just in this first quarter. Due to the travel bans and the general disinclination to travel at the moment, US tourism from Chinese visitors will take a compounding hit in addition to the losses from the ongoing trade war with China. Relatedly, global airline revenues are predicted to drop by $4-5 billion in the first quarter of 2020 due to flight cancellations. Automobile makers are closing plants in China as the much-needed inputs such as steel and aluminum are shrinking the availability of parts. As ground zero, China is suffering the most so far. China’s growth rate is expected to drop from 6% to 4.5% in the first quarter of 2020. As the infection sweeps through the Chinese labor force, factories are shutting down or lowering output capacity, slowing the flow of parts and final products from China. Virtually all countries are and will be impacted by the break in the supply chain as a result of reduced output from China. The absence of a single small component may render a final product unachievable. As supply falters across various sectors and products reliant on Chinese manufacturing, we should anticipate a rise in those prices. On the other hand, China is one of the largest markets for US products, especially Apple electronics and fashion items, so we should anticipate a significant decline in demand from that large consumer base as spending shrinks among the Chinese population. The Severe Acute Respiratory Syndrome (SARS) outbreak in China in 2003 provides a rough analogue on which to base predictions of the economic impacts of COVID-19. Virulence was highest from November 2002 to July 2003, and that nine month period was all the time needed for the disease to infect almost 8,500 people and kill over 800 people globally. Lee and McKibbin estimate the total economic cost of the 2003 SARS epidemic to be around $40 billion. The geographic dissemination of COVID-19 is currently akin to that of 2003 SARS with cases concentrated in China and small clusters popping up in Asia, Australia, Europe, and North America. The COVID-19 mortality rate is much lower at 2% versus 10%; however, the total number of coronavirus cases after just a couple months greatly surpasses the total case count for SARS at over 75,000. Though the loss of life may, thankfully, be much less severe with COVID-19, the adverse economic impacts of this outbreak may greatly surpass that of SARS. In 2020, we are more of a global economy than in 2003 and supply chains for a cornucopia of products are spread across nations and even continents, so a kink in one place catalyzes a domino effect across borders and industries. Unfortunately, there is no end in sight for COVID-19 as we approach March; therefore, the hits to the global economy will continue to spread across sectors and countries, as well as grow in severity. Only time will tell the full scale and spectrum of adverse economic effects instigated by COVID-19.
The 2021 Nuclear Weapons National Security Budget Proposal
The 2021 budget proposal exemplifies the continuing shift in the US nuclear posture toward a renewed nuclear arms race. This month, President Trump sent Congress a proposed Fiscal Year 2021 budget request of $740.5 billion for national security, 95% of which is for the Department of Defense. The clear priority of the proposed budget is the expansion of investment in and capabilities of US nuclear weapons. The proposal requests almost $29 billion, a 16% increase from the previous year, for the modernization of the US nuclear weapons arsenal. In addition to the $29 billion for modernization, the proposal includes other related items that would bring the total nuclear weapons budget to about $50 billion. The bump in nuclear weapons investment comes at the cost of shrinking most other security and defense programs. This should come as no surprise given Trump’s proclivity for nuclear strength as evidence by his late 2016 tweet, “must greatly strengthen and expand its nuclear capability until such time as the world comes to its senses regarding nukes.” Despite recommendations that DOD dedicate more resources on challenges from strategic rivals, namely China and Russia, the proposal outlines cuts to such programs. For example, the Navy is preparing for a significant reduction in funding for new warships. Lawrence J Korb, former Assistant Secretary of Defense for Logistics and Materiel Readiness, recommends that the administration extend the New Strategic Arms Reduction Treaty (START) with the Russians and resume negotiations. This would renew efforts toward reducing nuclear arsenals and enable the allocation of limited resources to programs that make our country and the world safer.
GAO Report – National Biodefense Strategy
The Government Accountability Office (GAO) has released a new report – “National Biodefense Strategy: Additional Efforts Would Enhance Likelihood of Effective Information”. You can access it here, but the report notes that “There are a number of challenges, however, that could limit long-term implementation success. Among other things, there was no documented methodology or guidance for how data are to be analyzed to help the enterprise identify gaps and opportunities to leverage resources, including no guidance on how nonfederal capabilities are to be accounted for in the analysis. Many of the resources that compose national capabilities are not federal, so enterprise-wide assessment efforts should account for nonfederal capabilities.” Moreover, the report points out that agency officials struggled to identify how decisions were made and there generally lacked a clear process or series of roles for joint-decision making, “As a result, questions remain about how this first-year effort to catalogue all existing activities will result in a decision-making approach that involves jointly defining and managing risk at the enterprise level.”
Pandemics and Podcasts
There are a lot of great podcasts in the infectious disease and biodefense world, so we’ll be spotlighting a few from time to time. Our first is the Next Generation GHS episode from last week, in which GMU Biodefense MS alum Jessica Smrekar sat down to discuss COVID-19. You can listen to it here. Jessica noted that “It was great sitting down with Jono and Taylor to hash out this rapidly developing COVD-19 outbreak in light of Jono’s book, The End of Epidemics: The Looming Threat to Humanity and How To Stop It. We discussed at length the weak links in local, national, and international health structures that leave us vulnerable to disease outbreaks and how we can remedy these in the future. Jono’s book outlines 7 specific actions that, if taken, could reduce these gaps and allow us to create a safer world. We explored the problems we face in developing strong, resilient health systems and how these actions work to solve those problems. Though the COVID-19 outbreak really highlights that we are not where we should be to keep our world safe, Jono expressed ‘the NextGen Group and your leadership and the fact we have such a mobilized network worldwide makes me optimistic. I think we’re building a really powerful network, both internationally and at the national level. And it’s that network of capable, informed, engaged people, who really do care about having a safer world, I think that’s what makes me feel optimistic’.”
 News of the Weird
News of the Weird
Video games and outbreaks – apparently they go hand in hand. Virus games are growing in popularity right now, in the middle of the COVID-19 outbreak, especially that of Plague, Inc. “Plague Inc. and Pandemic may have a certain morbid appeal in the time of the coronavirus. But they have more than that to offer, many experts and players agree. ‘I can certainly understand the hesitation around this — no one wants to trivialize the very real human suffering that this coronavirus has brought with it,’ said Leacock, Pandemic’s creator. ‘But the reality is that playing helps us process the world around us, and people may be turning to these games now for that reason’.”
Outbreak Dashboard
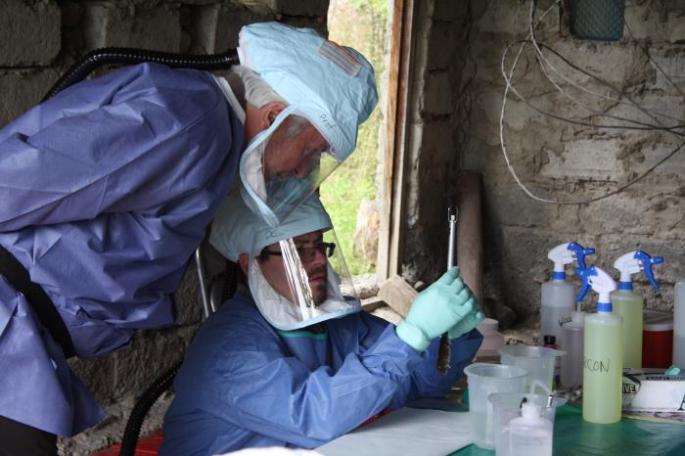
Qatar has reported a new MERS-CoV case, marking the fourth case since December. The DRC outbreak of Ebola has now reached 3,443 cases with over 330 suspected cases under investigation.













 SynBio Salmagundi:
SynBio Salmagundi: 









