Happy Friday! As we close out the month of July, Texas has reported its first local case of Zika in 2017. If you’re not convinced about the threat of antimicrobial resistance, check out this video on the ability for bacteria to resist even new antibiotics.
The Reality of Trump’s R&D Cuts
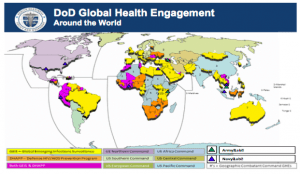
There’s been a steady stream of reports regarding the hits to global health spending that the new administration is making. The proposed 2018 “A New Foundation for American Greatness” budget hits financing of global health security, which is already poorly funded. While Bill Gates met with president Trump several times in efforts to persuade him of the importance of investing in global health and the R&D that goes into it, it seems that the continued assaults to funding aren’t going anywhere. A recent report by the Global Health Technologies Coalition and the Policy Cures Research of Australia took a different approach to swaying the president – money and fear. “The report explains that between 2007 and 2015 an investment of $14 billion (£10.7bn) in global health R&D resulted in a $33 billion injection back into the economy and the creation of 200,000 jobs. Spending since 2000 resulted in 42 successful products, including 11 for malaria and ten for TB. Want to ‘Make America Safe Again?’ Start by investing in R&D.” Just like the Nuclear Threat Initiative highlighted last week in their focus on the GHSA and importance of investment in global health, this report drives home the economics of global health security. We know that an outbreak anywhere is an outbreak everywhere, but for many, it can be difficult to see that when we’re not experiencing a major outbreak on American soil. Despite the impact of Ebola cases in the U.S. in 2014, the rise of antimicrobial resistance, and growing concerns regarding dual-use research and biosafety, there is a consistent struggle to truly get support for not only global public health, but also the R&D that supports biodefense efforts. The report notes that “Between 2007 and 2015, the US government invested nearly US$14 billion dollars in R&D for global health. In comparison, in 2015 alone, the US government spent $1.05 trillion on Medicare and health, $609 billion on the military, and $102 billion on education. Despite relatively limited investment, US government support was essential in helping advance 42 new technologies approved since 2000 – including 11 new products for malaria, 10 for tuberculosis (TB), and 1 for HIV/AIDS.” The U.S. is not an island – we rely on global cooperation and R&D alliances to help fight off current and future microbial threats. Global health security means that we must invest in efforts at home and abroad and to decimate an already limited budget for such efforts would have worldwide ramifications. FYI – the DoD released their guidance on global health engagement (hint: global health cooperation and engagement is important).
Worry About Water Bugs, Not Sharks
While everyone is up in arms about Michael Phelps not really racing a great white shark, some are saying, “hey…there’s actually a lot of microscopic water germs that are way scarier!” “You’re 75 times more likely to be killed by lightning than by a shark. On average, one person dies of a shark attack every other year in the United States.” The real danger rests in our love of water activities during the summer, whether it be a public pool, water park, private pool, or lake. FYI, I’ve seen one too many presentations on outbreaks associated with splash pads…they are diarrheal disease hotspots. Here are some of the bugs you should actually be worried about in water – crypto, pseudomonas, shigella, legionella, norovirus, cyanobacteria, and the brain-eating amoeba Naegleria fowleri. How can we dodge these party-crashers? Avoid swallowing the water…don’t go swimming if you’ve had diarrhea recently, check those chlorine and pH levels, and make sure to rinse off from time to time.
 Emergent Biosolutions Goes On A Spending Spree
Emergent Biosolutions Goes On A Spending Spree
While the future of global health R&D is a little bleak, Emergent Biosolutions is sprinkling some funding around to expand its drug portfolio. “Five days after the company agreed to pay $97.5 million to acquire the smallpox vaccine assets of pharmaceutical giant Sanofi it handed another $96 million to GlaxoSmithKline, one of biggest healthcare providers in the world, to acquire raxibacumab, an antibody that treats a form of anthrax that can be inhaled. Both deals are part of a broader expansion plan that Emergent’s executives hope will turn it into a $1 billion-a-year company by 2020.” These investments are more in the direction of defense against high-consequence biothreats, and their Chief Executive, Daniel Abdun-Nabi, is pointing to not just nefarious biological events, but also those related to climate change. Abdun-Nabi notes that “There’s a real worry starting to grow across the globe about the re-emergence of pathogens that we might not have seen for a number of years,”.
Infection Control vs. MERS
Not surprisingly, infection control failures are a big source for MERS-CoV transmission. Despite ongoing outbreaks and training on PPE and isolation precautions, there’s a pretty significant trend in healthcare – poor infection control practices. A recent WHO report revealed the findings of a risk assessment regarding 199 MERS cases in four countries. Since December, 1/3 of MERS cases have been linked to healthcare facilities and while initial signs and symptoms are non-specific, they found that simply improving standard precautions (also known as universal precautions) could make a difference. Using basic infection control practices, like putting a mask on a patient with a cough, or utilizing isolation precautions when caring for a febrile patient, are all easy and critical components to preventing the spread of disease. “How MERS-CoV spreads in hospitals still isn’t clear and is the topic of scientific studies. The WHO, however, said observations suggests transmission occurs before infection prevention and control steps are applied and patients are isolated. The agency added that hospital outbreak investigations suggest that aerosolizing procedures done in crowded emergency department or medical wards without adequate control measures may have led to human-to-human spread and environmental contamination.” This is an interesting finding for several reasons. Firstly, infection control steps should be applied the second a patient walks into a healthcare facility. During measles outbreaks (and influenza season), many hospitals put kiosks in the hospital entrance that contain alcohol-based hand sanitizer and masks, with signs highlighting the importance of such practices and to wear one if you have a cough. Secondly, utilize your triage staff. Either isolate or ask patients to wear masks during their triage process to prevent the spread of infection. We often wait until patients are in rooms to use PPE but the truth is that it can start a lot earlier. Also, emphasizing hand hygiene from the beginning can be monumentally helpful for everyone involved in patient care. Yes, healthcare workers are a significant part of the transmission chain, but visitors and the patients themselves play a big role. Overall, this study draws attention to infection control failures however, these aren’t new for those of us working in healthcare, and MERS is just a good example of how we can improve them. Preemptively isolating a patient won’t hurt, but delayed isolation can kill.
First Human Embryos Edited in U.S.
Researchers in Oregon are now the first team to attempt creating a genetically modified human embryo in the U.S. “The effort, led by Shoukhrat Mitalipov of Oregon Health and Science University, involved changing the DNA of a large number of one-cell embryos with the gene-editing technique CRISPR, according to people familiar with the scientific results.” Such work has not been previously done in the U.S. and Mitalipov’s team has shown it can be successful. While the embryos weren’t allowed to develop past a few days and there were never intentions of implantation, the altering of DNA codes within human embryos is a significant leap for biotechnologies like CRISPR. While many highlight concerns with the future of such work and the risk of “designer babies”, the NAS report in February has been seen as a green light to test germline modification. “The advisory committee drew a red line at genetic enhancements—like higher intelligence. ‘Genome editing to enhance traits or abilities beyond ordinary health raises concerns about whether the benefits can outweigh the risks, and about fairness if available only to some people,’ said Alta Charo, co-chair of the NAS’s study committee and professor of law and bioethics at the University of Wisconsin–Madison. In the U.S., any effort to turn an edited IVF embryo into a baby has been blocked by Congress, which added language to the Department of Health and Human Services funding bill forbidding it from approving clinical trials of the concept.”
MSF Lessons Learned During the DRC’s Recent Ebola Outbreak
There have been dozens of analyses since Ebola burned through West Africa in 2014/2015 however, a latest report from Médecins Sans Frontières/Doctors Without Borders (MSF) is providing insight regarding the 2017 outbreak in the Democratic Republic of Congo. The small outbreak (which seems odd to say about a disease like Ebola, but that was until 2014) resulted in the deaths of four people in a remote part of the DRC. When news first sprung up that cases were identified, the world waited with bated breath as the memories of the the last horrible outbreak were all too fresh. Fortunately, rapid field team and resource deployments aided in the quick response that halted the disease in its tracks. MSF was a part of such efforts and since the outbreak was declared over, they have identified five major lessons. Firstly, train frontline health workers. This one is music to my ears, especially in terms of the poor infection control practices among healthcare workers that made them 21-32 times more likely to acquire the diseases. “Healthcare workers play a crucial role not only for the health of the people they serve directly, but also for general epidemiological surveillance for outbreaks like Ebola, but also for more common deadly infectious diseases such as measles and cholera. A health system cannot rely on just one person to play the crucial role of on-the-ground surveillance. What is needed are proper surveillance systems in resource-poor countries, which were clearly lacking in West Africa at the beginning of the epidemic.” Secondly, a forgotten disease finally taken seriously – this is all too true in that many did not know of Ebola until it sent shockwaves through West Africa. Now, the disease is top of the agenda and rapid mobilization is triggered. Third, back to basics, which means that while we can focus on vaccines and new drugs, we can’t forget the basic pillars of outbreak control, like surveillance, isolating and treating the sick, looking for new cases, contact tracing, burying the dead safely, and engaging and mobilizing the local community. Fourth, location matters. The recent outbreak occurred in a very remote and forested area, which impacts movement of contacts, as well as acquisition of supplies. “As in all previous outbreaks before West Africa isolation played a key factor for the containment of the virus.” Lastly, medical interventions are not the magic bullet. “MSF was willing and actively preparing to use the Ebola treatments that are still in development. However the outbreak was over before the process to allow the use of experimental products was complete, so none could be used this time. This outbreak however acted as a booster to speed up the process of preparing medical protocols so that new drugs, still in the experimental phase, can be used in a way that is as safe and ethical as possible.” In the end, the rapid control and early response measures, coupled with the limited size of the outbreak, helped prevent its spread before the vaccine could even really make a difference.
Global Catastrophic Biological Risks Definition – Center for Health Security
The Johns Hopkins Center for Health Security released their working definition for global catastrophic biological risks (GCBR) in efforts to draw attention to this special category of global threats and focus future efforts to combat them. The definition is: “Those events in which biological agents—whether naturally emerging or reemerging, deliberately created and released, or laboratory engineered and escaped—could lead to sudden, extraordinary, widespread disaster beyond the collective capability of national and international governments and the private sector to control. If unchecked, GCBRs would lead to great suffering, loss of life, and sustained damage to national governments, international relationships, economies, societal stability, or global security.” You can read the article and ten commentary pieces written by a variety of leading scientists and public health experts here.
 How Infectious Diseases Shape Culture
How Infectious Diseases Shape Culture
When we think of infectious diseases, we tend to imagine morbidity and mortality. While this is accurate, there’s a lot more that these microbes impact, like language, culture, etc. We know that during the European bubonic plague in the 14th century, urbanization and economic development were slowed, but those skilled laborers who survived were highly valued. Consider even the food we eat, which has several cultural dynamics within it. We avoid raw meat, raw milk, and even stopped eating raw cookie dough or cake batter (ok, let’s be honest, we still lick the bowl, right?). “Many words and expressions commonly used in English have origins linked to an infectious disease. One such common phrase, used for a person who may not have symptoms of an infectious disease but can transmit it, is to call them a Typhoid Mary. In 1906 Mary Mallon, a cook, was the first healthy person identified in the USA as a carrier of the typhoid bacilli that causes typhoid fever, a serious disease for the Western world in the 19th century (but which globally exists and has often existed in poor communities).” Consider even the term, “feeling lousy”, which originated in conjunction to those with lice who became anemic and experienced general malaise. “In the late 1880s Tunisia experienced severe infectious disease epidemics of cholera and typhoid, and famines, which so badly depleted its economy that it was unable to pay off its debts. This made it vulnerable to French occupation and then colonisation.” There’s been a substantial body of literature that looks to the security implications of disease and how it may leave countries open to political and military disputes (check out Andrew Price-Smith’s Contagions and Chaos). The recent outbreak of Ebola has even changed the way American healthcare handles preparedness. Long thought a rare disease that we would never see, hospitals around the country now have Ebola Response plans and work to train front-line staff in case an outbreak occurs again.
Reports of Pediatric Deaths Following UN Sanctions Is Untrue
A recently article in BMJ Global Health is highlighting the fictitious statements made by Saddam Hussein’s government during the UN sanctions in 1990. “The United Nations Security Council imposed the sanctions in 1990 following Iraq’s invasion of Kuwait. The sanctions remained in place after the Iraqi army was expelled, on the grounds that Iraq’s weapons of mass destruction would need to be destroyed before they could be lifted. The sanctions greatly restricted Iraq’s ability to export oil and therefore to import supplies of food and medicines, prompting international concerns that the country’s children were being particularly hard hit.” Following these sanctions, a 1999 national survey was conducted by UNICEF and the Iraqi government, which reportedly found that “children in the centre and south of the country were dying at over twice the rate of 10 years earlier”. These results were used by several outlets for either support or refusal to invade Iraq. The researchers in BMJ Global Health have found that the results were “a deception” and studies done since 2003 have found no evidence of such high rates. The researchers concluded that “The rigging of the 1999 Unicef survey was an especially masterful fraud. That it was a deception is beyond doubt, although it is still not generally known.”
Stories You May Gave Missed:
- CARB-X Awards $17.6M To Fight Global Antimicrobial Resistance – the private initiative, CARB-X, was established with the purpose of facilitating global efforts to combat antimicrobial resistance. This week they announced $17.6 million will fund research efforts by scientists in India, Ireland, France, Switzerland, the U.S., and the U.K. “The seven supported projects include five potential antibiotics targeting Gram-negative bacteria, a new treatment for drug-resistant gonorrhea, a new drug molecule that targets resistance in cystic fibrosis infections, and Phase I development of an oral, broad-spectrum antibiotic. The latest round of awards is part of a $455 million commitment by the U.S. Government and the Wellcome Trust over five years. The first 11 projects to receive funding were confirmed in March, and additional funding announcements are expected later this year.”
- Biodefense World Summit – If you missed this event in June, check out some of these highlights that include talks on pathogen detection, food safety, and the importance of biodefense in the U.S.!
- Papaya-linked Salmonella Outbreak – Just went you thought it was safe to go back to the summer fruit salad…. Sadly, salmonella is a current risk for papaya-lovers across the U.S. as an outbreak of Salmonella Kiambu has sickened 47 people across 12 states. “Most of the cases were reported in five eastern states: New York (13), New Jersey (12), Virginia (6), Maryland (5), and Pennsylvania (4). Seven states across a wide swath of the country, however, have each reported 1 case: Iowa, Kentucky, Louisiana, Massachusetts, Minnesota, Texas, and Utah. So far, 12 people have been hospitalized. The death involved a person from New York City. Illness onsets began May 17, with the most recent on Jun 28.Patient ages range from less than 1 year to 95 years, with a median age of 27. About two-thirds are female, and, of 31 patients with available information, 18 (58%) are Hispanic. The epidemiologic and lab investigations both point to tainted papayas as the source of the outbreak. Interviews with 25 sick patients found that 11 (44%) had eaten papayas, a significantly higher proportion of papaya consumption than in healthy Hispanic people (16%) interviewed around the same time.”



 This past Saturday (Earth Day), cities around the world saw hoards of scientists and supporters of research marching to both celebrate science, but also push for the preservation of funded and publicly communicated research. “The March for Science is a celebration of science. It’s not only about scientists and politicians; it is about the very real role that science plays in each of our lives and the need to respect and encourage research that gives us insight into the world. Nevertheless, the march has generated a great deal of conversation around whether or not scientists should involve themselves in politics. In the face of an alarming trend toward discrediting scientific consensus and restricting scientific discovery, we might ask instead: can we afford not to speak out in its defense?” Cities like Chicago saw 40,000 participating in the march, armed with lab coats, pink knit brain hats, and
This past Saturday (Earth Day), cities around the world saw hoards of scientists and supporters of research marching to both celebrate science, but also push for the preservation of funded and publicly communicated research. “The March for Science is a celebration of science. It’s not only about scientists and politicians; it is about the very real role that science plays in each of our lives and the need to respect and encourage research that gives us insight into the world. Nevertheless, the march has generated a great deal of conversation around whether or not scientists should involve themselves in politics. In the face of an alarming trend toward discrediting scientific consensus and restricting scientific discovery, we might ask instead: can we afford not to speak out in its defense?” Cities like Chicago saw 40,000 participating in the march, armed with lab coats, pink knit brain hats, and  Summer Workshop on Pandemics, Bioterrorism, and Global Health Security
Summer Workshop on Pandemics, Bioterrorism, and Global Health Security
 NSABB Meeting on DURC and Other Hot Topics
NSABB Meeting on DURC and Other Hot Topics



 Help stop the chain of infection by celebrating Infection Prevention week from October 16-22! Believe it or not, you don’t have to be a healthcare worker to stop the spread of germs. On antibiotics? Take them as recommended and finish your dose! Visiting the hospital or being admitted? Ensure you and your visitors wash their hands and avoid visiting ill patients if you’re sick. There’s a lot we can do to prevent the spread of infection and fight the battle of the bug, so make sure to check out how you can get involved!
Help stop the chain of infection by celebrating Infection Prevention week from October 16-22! Believe it or not, you don’t have to be a healthcare worker to stop the spread of germs. On antibiotics? Take them as recommended and finish your dose! Visiting the hospital or being admitted? Ensure you and your visitors wash their hands and avoid visiting ill patients if you’re sick. There’s a lot we can do to prevent the spread of infection and fight the battle of the bug, so make sure to check out how you can get involved!

 GMU Biodefense Graduate Program Informational Videos
GMU Biodefense Graduate Program Informational Videos


 The U.S. Department of Health and Human Services has awarded
The U.S. Department of Health and Human Services has awarded