by Alena M. James
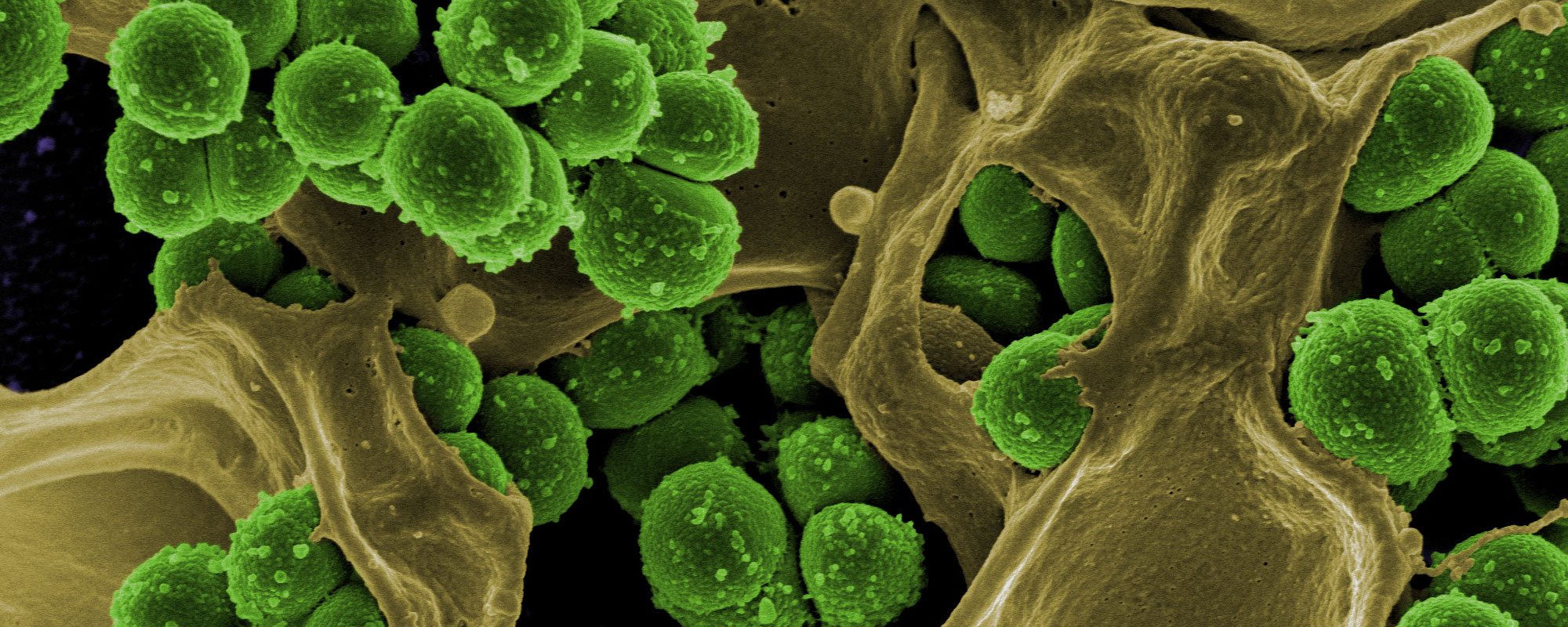
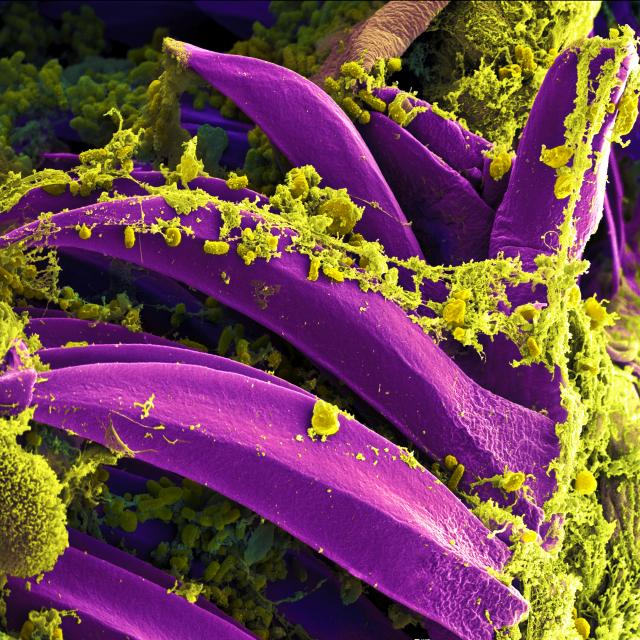
Yersinia pestisis a gram negative, bacillus shaped bacteria that prefers to reside in an environment lacking oxygen (anaerobic). It is typically an organism that uses the process of fermentation to break down complex organic molecules to metabolize. However, the organism is commonly referred to as being a facultative anaerobe, because it can live in the presence of oxygen and undergo respiration to generate energy for its cell. Its facultative capability is one reasons the organism can induce infection in highly oxygenated lung tissue.
This organism, primarily a zoonotic pathogen, has been held responsible for causing the bubonic form of plague responsible for the Black Death, the 14th century event that lead to the death of millions of Europeans. For years, the cause of the Black Death Plague pandemic has been linked to fleas. In much of Europe at this time, unsanitary living conditions provided the perfect breeding grounds for flea infested rats to flourish; while the fleas served as the perfect arthropod vector for Y. pestis to flourish.
The route of transmission of Y.pestis, from fleas to humans, was thought to occur via the urban cycle—when an urban rat becomes infected with fleas from a wild animal. Crowding in cities, poor hygiene, and unsanitary living conditions attracts large rat populations to the area. When a flea carrying Y.pestis bites a rat, the rat becomes sick and dies. No longer able to parasitize the rat, the flea moves from the rat to a new host. In crowded cities, the fleas from the dead rat will jump to humans to feed. When the flea bites the human it releases Y. pestis into the human’s cardiovascular system. Once in the cardiovascular system, the bacterial organism makes its way to the lymph nodes. There it replicates and spreads throughout the body causing septicemia. As Y. pestis proliferates within the lymph nodes it also forms hemorrhagic necrosis throughout the body. Painful swelling arises and the definitive painful symptom, the bubo,appears. After infection, a patient develops a high fever and the organism can target specific organs of the body like the lungs, liver, and spleen. Without treatment, a patient has a 75% mortality rate.
Last week, British scientists performed comparative DNA analysis on bacterial samples collected from 25 excavated skeletons found in the Clerkenwell area of London. These remains dating back to the 14th century contained samples of Yersinia pestis, the bacteria responsible for the Black Death. In an attempt to evaluate the virulent nature of the pathogen, the Y. pestis DNA collected from these remains were compared to DNA from the Y. pestis responsible for the deaths of more than 30 people in Madagascar back in December 2013. Researchers concluded that the DNA of both organisms revealed a high percentage of similarity and that the pathogenic nature of the 14th century Y. pestis is no more powerful than the Y.pestsis responsible for the Madagascar killings.
After considering this information and examining the plausible death of the skeletons, scientists believe that the fast-acting killing capabilities of Y.pestis are only likely to take place through airborne transmission. This conclusion undermines the urban cycle transmission method and suggests that the Black Death was mostly caused by pneumonic plague and not bubonic. British scientists are determined to examine more modern cases to confirm this new hypothesis. If confirmed, we may see pneumonic plague identified as the causative agent for the 14th century plague pandemic thus altering our historical account of the Black Death.
For British scientists, the transmission of Y. pestsis through respiratory droplets is a much more likely scenario for achieving rapid kills versus the urban cycle transmission method. Bubonic plague is not infectious and there is no human to human transmission from the buboes that form. However, pneumonic plague can be caused by bubonic plague if the Y. pestis pathogen makes its way via the lymph nodes to the lungs inducing infection. While in the lungs, the organisms are caught in respiratory droplets and are then disseminated into the air when an infected person sneezes or coughs. This quickly makes the host very infectious and a threat to those not yet infected. The mortality rate for patients suffering from pneumonic plaque without treatment is 100%.
Image Credit: crossrail.co.uk